The best and most beautiful things in the world cannot be seen or even touched – they must be felt with the heart. ~ Helen Keller
Rev Kane’s Wild Ride: What Open Heart Surgery is Like
Today I wanted to write about my experience of going through open-heart surgery. The exact surgery I had was a biological replacement valve implanted to replace my aortic valve. I was born with a birth defect, a bicuspid aortic valve. Essentially your aorta should have three leaves, two of mine had fused together leaving me with two instead of three and this narrows the opening and causes problems with the heart. Additionally, this condition, along with my high blood pressure caused additional pressure on my arterial walls leading to both an ascending aortic aneurysm and a smaller root aneurysm on top of the aorta. The video below explains the conditions, details of survivability etc… and the procedure to repair them. The repair I had, will hopefully last ten to fifteen years before I would need another procedure.
I’ll be honest, the procedure is a bit terrifying. The idea that they would be stopping my heart for a couple of hours. The idea of having my chest opened, my breastbone cut in half and being essentially split open like a lobster is not something I was looking forward to having done to me. However, it was a necessary procedure that should give me a better quality of life.
One of the things I didn’t completely expect, I hadn’t had major surgery before, were all of the pre-surgery tests and appointments, and man there are a lot of them. You of course meet with your cardiologist and the surgeon, but you also meet with an anesthesiologist, a surgical scheduler, a surgical nurse and a nurse practitioner. And it seems like just about everyone has a different set of questions and blood tests that need to be done. You also have to have a procedure, a heart catheterization where they feed a small wire up through an artery in your wrist or leg and into your heart to check for any blocked arteries, which determines whether or not you’ll need any bypasses during your procedure. Happily, I had no issues and no bypasses needed to be done.
In my case, my surgery almost got cancelled because my blood sugar numbers were too high, happily I was able to work with my general practitioner to get them into an acceptable range before surgery. Then, because there were two emergency admissions who needed surgery, my surgery was pushed back three weeks. It’s an odd thing I didn’t expect, they don’t absolutely confirm your surgery until the evening before. Which is crazy considering the night before you have eating restrictions and have to shower with specific surgical soap and wipe down your body with disinfectant wipes.
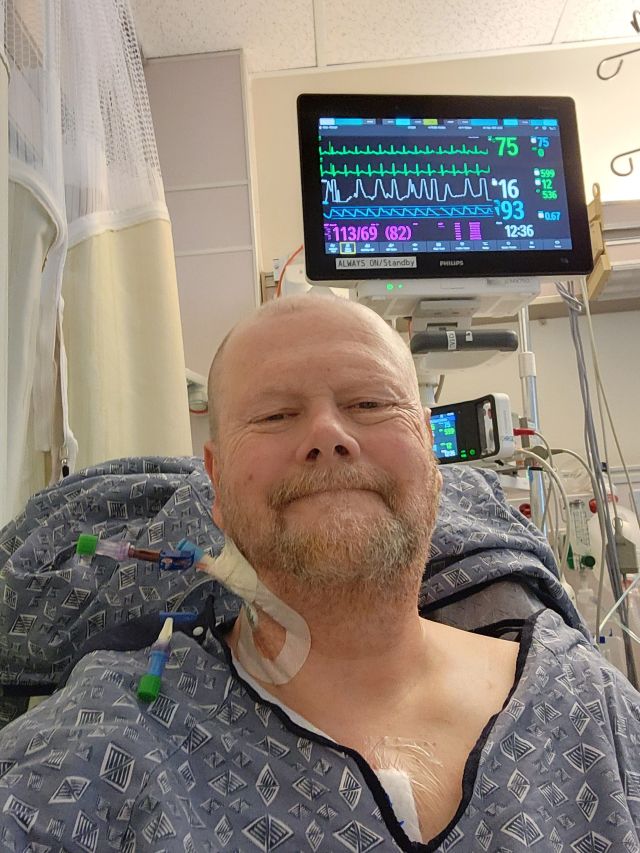
Happily, the night before they called about 6PM and confirmed me for the next morning. I of course had to arrive at the hospital at 6AM. The morning of surgery flies by pretty fast, you go through admitting and then walk up to the surgical floor waiting room. Once they pull you in they put you in a bed, strip you down to the lovely hospital gown, take your vital signs, ask you a bunch of questions, have you sign away your life (you hope not literally) and then stick an IV into your arm. They pretty quickly roll you down to the operating room staging area, here a person comes in and shaves any areas that need to be shaved. Then a little while later they roll you out into the hall, your doctor and team make a quick appearance and then you’re rolled into the operating room. The anesthesiologist says good morning, drops a mask on you and says take deep breaths, I remember taking two. Then, what feels like ten seconds later you hear the voice of a nurse saying, “Mr. Kane, you had heart surgery, it’s 3:30PM on the day of your surgery, you have a breathing tube in, when you wake up a little more we’ll get it out.”
A couple of quick things, what added to my level of trepidation prior to surgery was the experience some others have had. As a healthy person, survival rates for this surgery are near 99% but there’s always that 1%. I know three people who’ve had this surgery. A friend a couple of years ago who had the surgery and had multiple complications. My closest friend growing up, who had the surgery a year ago and died. And a colleague, who six months ago had the surgery came out and a few days later went into a coma for a time, he’s happily ok now. So I was afraid of dying of course and also of ending up in a coma. So one of the things I did was shave my beard real short, I was planning to touch my face when I woke up. If my beard was gone, or really long, I would know I’d been in a coma. But my magnificent nurse took that anxiety away by saying it was the day of my surgery, I was very grateful for that.
My second fear was the breathing tube. First, I was an asthmatic growing up, so one of my biggest fears is not being able to breathe, I’m also my grandfather’s grandson and at 90 he woke up from being unresponsive and ripped out his breathing tube, IV’s and catheter. I was really afraid of waking up with the breathing tube in my throat and had warned my team I might freak and rip it out. The anesthesiologist I met with pre-surgery had told me not to worry, most people didn’t even remember it coming out, a combination of all of the pain meds and sleep drugs. And in fact, later that night when I started to be a bit clear headed I really didn’t remember it.
Until the next day, you see the next night, in the next room another patient was going through the process, with the nurse I’d had the day before. Hearing her talk that patient through the process brought the full memory screaming back to me. It wasn’t as horrible as I had imagined, but it wasn’t pleasant. When I first woke up and could feel the tube I started to freak, the nurse put me at ease. I really didn’t like having the tube in, I bit down on it a couple of times and a couple of times gagged a little. But I was also still fading in and out of consciousness and they were instructing me to breathe deeply. I was concentrating on doing that and I think it took about a half hour before I heard my nurse say, “I think he’s ready.” They made the call to the respiratory person and then it was a process of breathing deeply then exhaling hard as they pulled it, unpleasant but it made me really happy. I fell in and out of consciousness for the rest of the night. Often listening to everyone but for some reason it was a couple of hours before I opened my eyes for the first time.
While you may anticipate some down time of just laying there recovering, they warn you in advance this will not be the case, they will have you up and walking the next day, and they do. The next morning I woke up with an IV in my arm, an IV in my neck, two drainage tubes coming out of my chest, two wires coming out of my chest hooked up to a portable, external pacemaker and of course the catheter. I actually didn’t mind the catheter, it was nice not to have to get up to go to the bathroom and there are a lot of fluids introduced into the body during surgery so the drainage tubes and catheter initially stay very busy. Then they pump you up with Lasix and the fluids rain out of you like a waterfall. But that first day, they did indeed get me out of bed for a short walk with a walker, while six different sets of tubes and wires hung from my body and we dragged an IV tree and a vital monitor around with us.
The biggest issue those first two days are the chest tubes, they hurt like hell. Every breath is a little pain, every big breath a lot of pain and when you cough it’s like people are stabbing you with serrated knives. I was on a lot of pain meds the first couple of days and it still hurt like hell, not to mention your chest isn’t all that comfortable either, and I have a pretty high pain tolerance. They tell you again and again, it will get better once the chest tubes come out, I would smile and say ok. Inside I was thinking you’re a bunch of lying bastards give me drugs.
I didn’t have much of an appetite at first, my first breakfast all I could eat was a small yogurt. I would eat about a third of my meals the first couple of days and experienced a really weird thing. I would in an instant get super hungry, but if i didn’t eat within about five minutes, I’d suddenly get nauseous and not want to eat anything. Eventually I learned to save a piece of fruit from each meal, so when my hunger hit, I could eat immediately.
On day three in the ICU they came to take out my chest tubes, it was the weirdest damn sound and feeling when they pulled them out. They pulled them out simultaneously and it made a weird squishy sound. The image I had was them pulling two large squid through a puddle of Vaseline with all the assorted squishiness that would command. But the nurses and doctors had not lied, literally the first breath after the tubes were out was pain free, it was an unbelievable and amazing difference. While it still hurt a bit to cough, I immediately was able to cut back on almost all of the pain drugs save the max dose of Tylenol that I was on. After the chest tubes I actually never took anything other than Tylenol for the next four days, nor since coming home.
The next two days in the ICU were the same routine wake up, eat, walk, nap, eat, walk, nap, eat walk sleep. I would have left the ICU a day sooner, but they didn’t have a bed for me downstairs on the step down floor. We dealt with lots of little things, BP at times too low, discovering I had sleep apnea, I don’t normally sleep on my back. They would as the days progressed pull the catheter and the neck IV and eventually pulling the pacemaker wires which was a really wild sensation. I think the idea that they were literally pulling these off my beating heart added to the exhilaration of the moment. When they do, your heart does this weird fluttery thing, I didn’t like it. I was lucky, they never needed to pace my heart, I didn’t have any complications like Afib, and there were no infections. The one big thing I had to overcome to get out of ICU was making a bowel movement. That happened on day three and when it did, it really did, I’ll spare you the details but it matched the name of a Robert Plant solo album.
While you’re in ICU you get visits from all sorts of specialized folks, social workers, rehab folks and physical therapy who assess your mobility and strength. They teach you out to get out of bed without using your arms and give you tips for recovery. They also take you on walks, happily I did well enough that they cleared me before I left the ICU which was great, but it also meant once I moved floors there was no way for me to walk stairs and I have twelve steps leading up to my apartment.
The step down floor was a very typical hospital stay, I got to take my first shower. Each day is routine which of course means they wake you up two or three times a night and you have a lot less attention than you did in ICU. I was happy to have good nurses, and this time is really all about them making sure there are no complications, you’re mobile and your vital signs are good. I left there in three days and my cardiologist told me I left the hospital faster than any of her other patients had before. I credit that to how much I prepared for the surgery, which I address in another post.
Finally, going home was stressful and exciting, I did the stairs easily. I did well, I expected the first week to be hell. The first couple of nights, sleeping in a recliner and on the couch weren’t great. I broke down and bought an adjustable bed on day 4, being able to sleep in my bed made everything better. Being home is mostly about patience. You need help the first couple of weeks (this assumes you were healthy and fully mobile and independent before surgery) there are just some things you can’t do. By week four it’s a lot better, it’s week nine for me right now and I’m finally feeling close to normal.
So, if you’re about to go through this, I hope this gave you some info and peace of mind, and good luck on your surgery and recovery. ~ Rev Kane
